
Get the Facts About Salivary Gland Tumors
Salivary gland cancers originate in the salivary glands. These glands are present in three major pairs and they are found below the jaw. There are smaller ones inside the cheeks and lips, in the throat and in the mouth. When tumors develop in these glands, they are usually in the parotid gland. In fact, about 85 percent of these tumors are found in this gland and approximately 25 percent of tumors in the parotid are determined to be cancerous. However, overall, tumors in the salivary gland are rare.
Causes
It is not fully understood what causes salivary gland tumors. However, it is known that when certain cells in these glands experience a DNA mutation that a tumor develops. The mutations make it possible for the cells to divide and grow rapidly. Normal cells would die, but the mutated ones continue living. They accumulate into a tumor and nearby tissues are invaded.
There are three known risk factors associated with these tumors. Older adults are most often affected, but they can develop at any age. Those who have been exposed to radiation either with medical treatments or in the environment are at a higher risk. People working in certain environments might also be at a higher risk, such as those working in asbestos mining, rubber manufacturing, and plumbing.
Symptoms
When symptoms occur, they are generally isolated to the area where the tumor is present. They may include:
- Swelling or a lump close to the site of the tumor
- On one side of the face, muscle weakness is possible
- Trouble swallowing
- Numbness of the face near the area of the tumor
- The affected salivary gland can be painful
- Difficulty opening the mouth wide for eating or examination
The symptoms can occur with tumors that are both cancerous and noncancerous. The severity depends on several factors, such as the size of the tumor and the patient’s overall health status.
Treatment Options
After a thorough examination process, determining if the tumor is cancerous and then staging a cancerous one, a treatment regimen is determined. Chemotherapy may be used for more advanced forms of salivary gland cancer. However, it is not considered to be a standard treatment.
Radiation therapy works to kill cancer cells using various high-powered energy beams. Following surgery to remove a tumor, this may be used to kill any cancer cells that may still be present. It may also be used instead of surgery when a tumor is too risky to remove.
Surgery is the most common treatment method. Smaller tumors may be removed alone or with the affected salivary gland. If the cancer has spread, nearby lymph nodes may need to be removed. In the most serious of tumor removals, reconstructive surgery may be needed.
Salivary gland tumors are not a health issue most people hear about unless they have experience with them. However, basic knowledge is important to protect a person’s health. Like all tumors, it is imperative to have them evaluated promptly. If it is determined that the tumor is cancerous, patients and their doctors will work together to build a treatment plan.

Recommendations for Pediatric Throat Surgery
Throat illnesses and conditions can afflict patients of any age. However, children are often at a greater risk of certain throat diseases because of their immature immune systems and also exposure to germs at school, camp, and other public places. When home and over-the-counter remedies have little to no impact on helping your child heal from throat conditions like tonsillitis, strep, sleep apnea, and swollen adenoids, it may be time to have your son or daughter undergo pediatric throat surgery.
What is Pediatric Throat Surgery?
As its name implies, pediatric throat surgery is a surgical procedure designed for and performed on patients under the age of 18. The surgery that your own child undergoes can be relatively minor and minimally invasive. It can also be rather extensive and require an overnight stay in the hospital.
Some of the primary pediatric conditions treated with throat surgery for children include:
- Tonsillitis
- Chronic strep infections
- Swollen adenoids
- Benign or malignant tumors in the throat
- Chronic pus pockets or tonsil stones
- Sleep apnea
The type of surgery that your own child will undergo will depend on the diagnosis of the throat condition as well as the recommendations of your son or daughter’s ENT surgeon.
Who is a Good Candidate for Pediatric Throat Surgery?
Pediatric throat surgery is typically reserved for children under the age of 18 who are in good overall health. Your child will be closely examined by the ENT surgeon. You also may be required to have your child examined by his or her primary care pediatrician prior to the operation.
This thorough pre-operative examination ensures that your child does not suffer from any illness or injury that could put him or her at risk during or after the surgery. Some of the conditions that could prevent your child from going through the surgery include:
- Chronic asthma
- Anemia
- High blood pressure
- Heart disease
- Kidney, liver, or other major organ
- Hemophilia
Otherwise, if your child does not suffer from any of these illnesses, he or she can undergo pediatric throat surgery and should be able to recover well from the operation.
What to Expect During the Surgery
As a parent, it is nerve wracking to entrust the care of your child to even the most qualified of surgeons. Still, you may have better peace of mind by knowing what will occur during the operation.
Your child will likely be sedated and put to sleep during the surgery. Sedation ensures that your child stays still and calm while the surgeon performs the operation.
The surgeon may also use laser technology or traditional surgical instruments like scalpels to remove the tonsils or adenoids or work on other tissues that contribute to your child’s throat condition. Depending on the invasive nature of the operation, your son or daughter may have stitches in his or her throat to close off the incision and prevent infection during the recovery period.
Recovery
Most children recover quickly with few complications from pediatric throat surgery. Still, you should know what warning signs to look out for as your son or daughter heals. Your doctor will want you to contact him or her if your child exhibits post-operative signs like:
- High fever
- Uncontrollable bleeding
- Difficulty waking or staying awake
- Excessive vomiting or diarrhea
- Allergic reactions like hives, difficulty breathing, or swelling of the throat
If your child does not exhibit signs of complications, it is still important for you to follow your doctor’s post-operative care instructions and to keep any post-op appointments with the surgeon. You may be encouraged to give your child pediatric pain reliever for pain and mild fevers.
You should also ensure that your son or daughter stays hydrated during the recovery period, which can last for seven to 10 days depending on the surgery that was performed. Your child should be kept out of school until the doctor clears him or her to return.
Benefits of Endoscopic Skull Base Surgery
Medical technology has transformed the manner in which doctors can now treat and perform head and brain surgery. They no longer are relegated to using invasive and painful means to treat patients for a variety of skull, sinus, or neurological conditions. Decide if endoscopic skull base surgery may be right for you and what benefits it can offer you as a patient.
What is Endoscopic Skull Base Surgery?
Endoscopic skull base surgery is a minimally invasive procedure that utilizes a lighted endoscope that is inserted through the sinuses to identify, target, and treat growths, injuries, and illnesses inside the skull cavity. Depending on the condition being treated, the endoscope may be angled to allow for better access to the injury or illness.
The endoscope is lighted to allow doctors to see clearly what structures and areas should be targeted during the surgery. It also may be used in conjunction with computer generated three-dimensional imagery to provide better pictures of the tumor or growth inside of the skull.
Because of the small size of the endoscopic equipment being used, this type of brain surgery is precise and comes with fewer risks than traditional brain surgery. It is less invasive and is faster from which to recover in many cases.
Endoscopic skull base surgery also results in less scarring and cosmetic damages to the patient’s appearance. Unlike traditional brain surgery, which typically requires extensive cutting and possible removal of some parts of the skull to reach the growth or tumor, this procedure does not compromise a patient’s appearance and is less painful.
As it becomes more commonly utilized in hospitals and medical facilities across the U.S., you may wonder which conditions can be treated with endoscopic skull base surgery. It now benefits more patients who otherwise may have had to undergo extensive and invasive operations to treat their illnesses or injuries.
Why is Endoscopic Skull Base Surgery Performed?
Endoscopic skull base surgery is performed to treat, remove, or minimize tumors or growths inside of the skull. However, it is also utilized to correct or lessen injuries or illnesses caused by congenital defects or accidents like falls or concussions.
Doctors also use in situations such as:
- Rathke cleft cysts
- Lesions
- Hormonal disorders
- Mucus secreting gland cancer
- Tumors in the dermoid, epidermoid, or pituitary gland
Moreover, it is now commonly utilized to address illnesses like:
- Chondroma
- Cushing’s disease
- Invasive fungal sinusitis
- Compression of the optic nerve
- Squamous cell carcinoma
Endoscopic skull base surgery can be performed on patients of all ages including children who otherwise may be disqualified from more invasive brain surgery.
Benefits of Endoscopic Skull Base Surgery
Endoscopic skull base surgery comes with numerous benefits that make it appealing to both surgeons and patients. It is minimally invasive, meaning that surgeons do not have to perform extensive cutting into the skull. It is also faster to perform and can be done within an hour or slightly longer depending on the condition being treated.
It likewise is less painful and requires less sedation or general anesthesia than traditional surgery. While it is typically performed in the hospital, patients do not need to check in for lengthy stays. Many patients can go home within one or two days after their surgeries.
Because it is less invasive, there is also a smaller risk of post-operative infection. The incision site will be closed with sutures or skin adhesive. However, the small size of the incision itself means that there is less of a chance of bacteria and viruses causing infection at the site.
This surgery results in little, if any, noticeable scarring. Most incisions are made inside of the nose or sinuses. Most patients recover their full appearances and suffer from little to no noticeable cosmetic changes. They remain confident in the way that they look and do not have to worry about others noticing any scars or deformities caused by the surgery.
Finally, endoscopic skull base surgery is faster from which to recover. Many patients are able to get back to their normal routines within a matter of days or weeks. They do not have to take a lot of time off from work or school to recover.
People who suffer from endoscopic skull base illnesses or injuries no longer need to go through extensive and invasive brain surgery. They now may be able to recover faster and better by undergoing endoscopic skull base surgery for cysts, lesions, tumors, and other conditions.
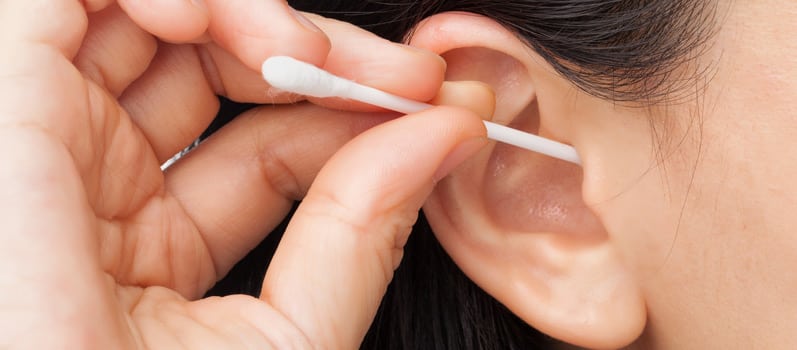
The Right Way to Clean Your Ears
Your body uses earwax (cerumen) to self-clean, protect, and lubricate your ear. The earwax that you may see on your ear is old and has moved to that spot after jaw motions, like chewing, transport it there.
As much as you may want to clean this earwax thoroughly, it takes careful steps to ensure that you do not damage your eardrum or affect your ability to hear.
What to Avoid
Contrary to popular belief, it is not recommended to stick a cotton swab inside your ear to clean it. This can actually push the wax in deeper and can damage your ears. In fact, blockage is one of the most common causes of hearing loss. Commercial ear candles should also be avoided, because they can contribute to burns, obstruction, or perforation of the ear.
What to Use
To clean your ears, wash the external part of your ear with a clean cloth. You can soften earwax blockage with a few drops of mineral oil, baby oil, or hydrogen peroxide. If you have trouble softening the wax or are prone to frequent bouts of impacted wax, contact your doctor. You may need to visit the doctor regularly to have the earwax removed.
Seeing a Doctor
You should see a doctor to evaluate your earwax if you experience any of the following symptoms:
• Hearing loss
• Itching
• Discharge
• Odor
• Earache
• Sensation of a plugged ear
To help remove earwax, your doctor may use an irrigation kit or a syringe technique with water and saline.








